Jonathan Spradley
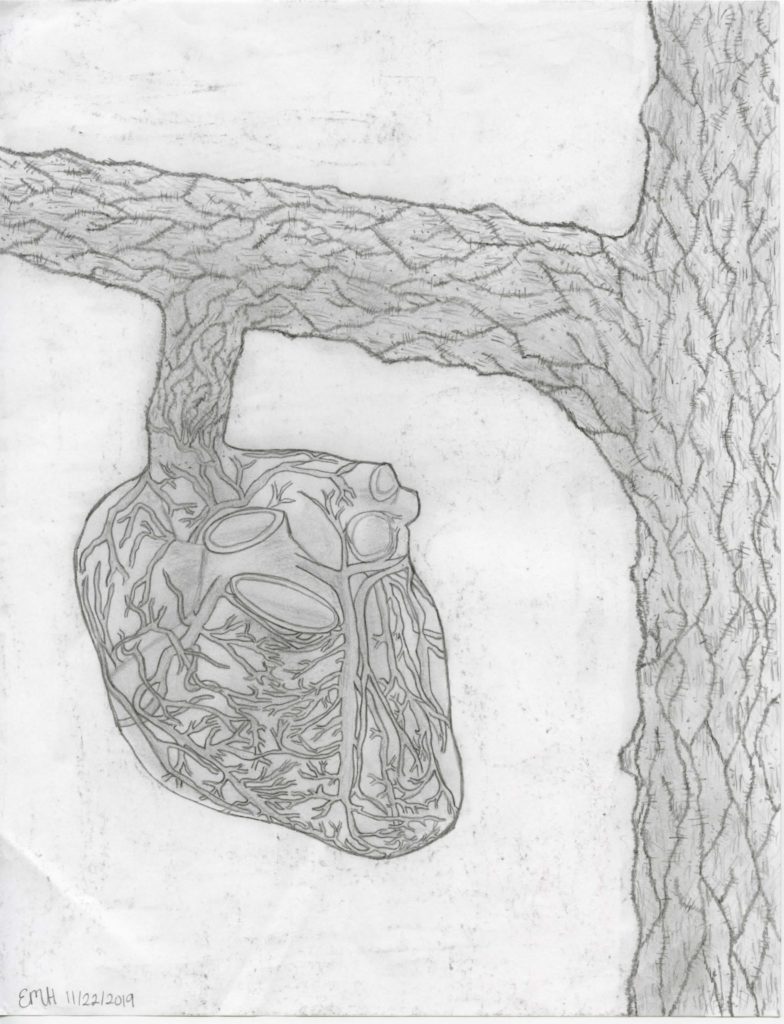
This image is a reminder of the intersectionality of healthcare disparities between geographic location and gender. Women, such as this one in Essaouira, Morocco, are tasked with difficult journeys of trying to participate in healthcare systems made inaccessible to them as doors are repeatedly closed in their paths.
Jonathan Spradley is a medical student at UAMS.